MedOrion’s Health Behavior Management Software shows how to predict tolerance levels in older adults and what you can do about it.
It is a known fact that older adults are more likely to have adverse drug reactions and there are valid, logical reasons for this. At the same time, deep learning is teaching us that there are dynamic hidden patterns in people’s behavior that either trigger action or raise the red-flag barriers when it comes to taking necessary medication.
Despite all we know, and for all that we are still learning, we tend to hang onto misconceptions when it comes to health behavior, especially when we’re trying to make sense of data without knowing the individual on a personal level.
For instance, we imagine that adults under the age of 70 would approach preventive care as their top priority in an effort to stay healthy and steer clear of potential health complications; After all, the 70s are the new 60s – who doesn’t want to stay healthy and strong? The majority of individuals in this group will argue that this is true, but when the question of medication tolerance comes up, many will admit that their capacity to ensure side effects falls short.
Prescriptions are abandoned halfway, changed during the treatment, and other times never purchased due to past experience with side effects. Despite all the good intentions members might have toward their health, the wisest experts in behavior change have always shared one golden rule: you can’t extinguish a bad or unsupportive habit, you can only change it with a better one.
Our team at MedOrion is constantly searching to break misconceptions related to health behavior. One of the insights that surfaced recently revealed:
“Members over 80 years of age are more likely to endure side effects for the value of the medication”
Why is the tolerance age so high?
Although side effects are a veritable obstacle to people’s lifestyles, members are willing to sustain the impact; they can look beyond the temporary discomfort of feeling ‘meh’ for a while for the chance to improve their health. Plus, they have already seen that taking their medication is what has curtailed any complications to their health thus far, even if they experienced unpleasant side effects.
What does this information tell us about other segments?
Surprisingly, members over 80 possess stronger willpower than younger age groups. Behavioral Science and AI experts analyzed the data and found that members under the age of 80 are more likely to search for alternatives before succumbing to acceptance.
Here’s the logic behind it:
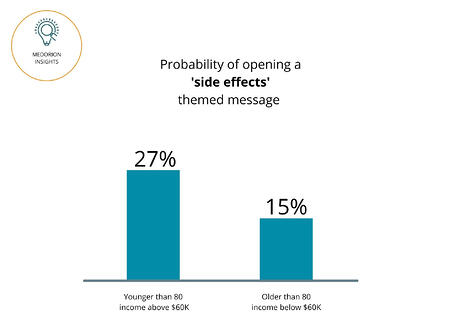
Members over 80 with an annual income below $60K are more likely to accept side effects of medication as expected, rather than something that requires further medical consultation.
Members under 80 with an annual income above $60K are more likely to actively seek medical help when they experience side effects, and maybe more aware of alternative prescription treatments. It is possible that higher income is a proxy for higher health literacy.
What does this mean for health plans?
Insights are powerful; they open doors of opportunity to act more accurately and use the right messages. Understanding why members are behaving the way they do offers invaluable pathways to success.
For the second segment – members over 80 with an annual income below $60K - the perceived or actual cost of consultation may deter them from requesting the service. In this case, a cost-focused message may be more relevant.
Based on these insights, members under 80 with an annual income above $60K are much more likely to be engaged with a message that encourages members who are experiencing side effects to consult with their physician and seek alternative treatment options. The incentives here from both sides are obvious.
MedOrion Insights
The Challenge with Members Under 80
They feel and look good, they’re active and perceive themselves as health-aware. While mental endurance and optimism go a long way to leading a long and happy life, there is another side to the coin, especially when dealing with members who are currently managing a chronic condition.
Forget Side Effects: They “Feel Fine”
They feel good and follow most of the guidelines, but they don’t fill the prescriptions on an ongoing basis. This is clearly a matter of lack of medication feedback.
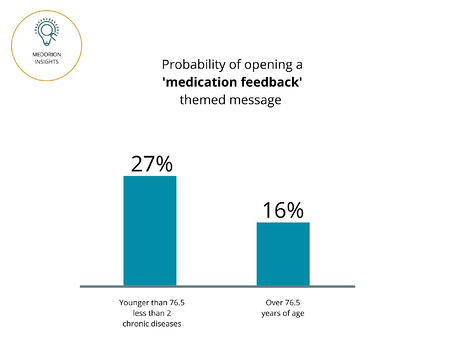
MedOrion’s insights show that members under the age of 76 with a single chronic condition are much more likely to be engaged with a message that details the importance of medication adherence and medication feedback.
Why? These members are more likely to skip or delay taking the medication due to the perception that they ‘don’t need it’ since they feel well.
What’s the best way to influence their health behavior?
It would be useful to pre-emptively target this population with an explicit message that questions the belief that they can skip medication if they feel fine. There are many ways to go about this.
For instance, you could explain that while the inner workings of the medication on the body may not be felt, the same goes for the potential damage of their chronic condition if left unaddressed. Or, there may be hesitations because a friend or relative took the medication and felt no change. Tapping into their concerns is critical to reverse the cycle.
MedOrion Insights
What does this mean for health plans?
Just like your members, you have more options than limitations.
Reaching out to members with a message that matters to them, and doing it consistently, gives you the advantage of building a relationship with each and every individual. Health Behavior Management AI and Behavior Science based platform provides you with the data you need to understand your highest value tasks to create these relationships.
More engaged members yield increased adherence to preventative health measures and improved member satisfaction; this change in members’ health behavior will also generate improved Star scores and lower operational costs as a result of reduced downstream expensive treatments.
Contact us to learn how you can use MedOrion’s Behavioral SaaS to improve medication adherence and feedback among your members and enhance engagement.
Click Here To Learn More About MedOrion
